This is a true birth story from the Northeastern U.S. It occurred in 2012. The name of the midwife has been changed in accordance with the mother’s wishes.
My first two babies were born, completely naturally and with no interventions, in a hospital with a fabulous CNM. They were both beautiful experiences. When I was pregnant the third time, my CNM had relocated to another state. I had been kicking around the idea of a homebirth for a long time, and since the only midwife that I trusted to provide a hospital birth that was up to my standards was gone, I decided to move forward with my homebirth plans.
When Susan walked into my house, she was not at all what I expected. She was young (my age, in fact) and exuded a natural air of serene confidence. She immediately made me feel at ease and was exactly what I was looking for: educated, competent, personable, and CRUNCHY. She patiently discussed every bulleted point on my checklist and answered every question thoroughly and to my satisfaction. I didn’t need to interview anyone else. I had found my midwife and I was excited!
My pregnancy was the most blissful nine months of my life. I spent it reading up on homebirth, doing prenatal yoga, getting frequent chiropractic adjustments, and chatting with my midwife during our very informal appointments. I received no testing or lab work of any kind. I longed for a boy after having two girls, so I did have one ultrasound to find out the gender. I was elated when the scan showed us a healthy boy!
My due date of February 9th came and went. I wasn’t worried, but my family became increasingly concerned. When I was over 41 weeks, my mom called to try to persuade me to go to a hospital for an induction. She said it wasn’t normal to go this far with your third. I rolled my eyes and wrote her concerns off as “fear mongering.”
When I was just one day shy of 42 weeks pregnant, I finally went into labor. My contractions became extremely intense very quickly. I told my husband not to call our midwife because I thought I was still early on in the process, but he called her anyway. An hour passed in waves of bone-crushing intensity and unfathomable pain.
I felt a release and called, “I think my water just broke!” from inside the pool. My midwife’s voice replied, “It looks clear. I see lots of vernix!” I looked up, startled; I hadn’t heard her come in. Just as I registered her presence, I felt an incredible urge to have a bowel movement. I summoned all the power and strength I had left to get out of the pool and head toward my bathroom.
I waddled to the bathroom and my entourage followed. I sat on the toilet and bore down. I was focusing all of my energy on relieving myself when Susan calmly said, “Just scoot your hips forward a little bit so that I can guide him so that his head doesn’t go into the toilet.” It took me a moment to absorb her words, and then it hit me: I was pushing! Just two hours before, I wasn’t sure if I was in labor. It hadn’t occurred to me that things had really progressed that quickly.
I was determined not to let my birth story include a toilet birth (and yes, I was thinking of my birth story while pushing!) so I got off the toilet and assumed the all-fours position. I pushed one time and his head was out. The time was called out, 4:15am. I was told that it would only be one more push and he would be here. I couldn’t believe how easy it was! Only two hours of labor, one push and I was almost done!
I pushed with all of my might. I pushed again and again, with all the force and determination of a seasoned natural birthing mama. It was then that Susan said in a very level tone, “You know that I would never direct you if it weren’t absolutely necessary. But this is important. I need you to do as I say right now.”
I did as she directed, assuming an array of positions: one foot up on the edge of my tub while squatting, back on all fours, etc. All the while I was pushing as though our lives depended on it. It dawned on me what felt so different: as I pushed, I didn’t feel any give. He stayed put, half born. He was stuck in limbo and I felt like I was pushing against a brick wall. I pushed and I pushed and I grunted, groaned and screamed. The pain was all consuming, beyond what I have ever felt in my life.
The situation was becoming grave. I saw it in the eyes of my husband and my midwife Susan. Terror was all over the face of her apprentice who had just arrived; she stood in the doorway, white as a ghost, shaking. It had been too long. My boy had to come out NOW if he had any chance of survival.
I felt a primal urge to stand up, so I put my arms around my husband’s neck and stood to push with every ounce of motherly determination I had in me. Susan had to reach deep inside my body to hook my son’s armpit and dislodge his shoulder from under my pubic bone where it had been stuck. The pain was breathtaking.
And then, relief! He was out! I had done it. 4:26am. Had it really only been eleven minutes since his head emerged? I had fought the battle of my life in only eleven minutes. Susan quietly said to her apprentice, “Go ahead and call.” I didn’t know who they were calling, or why. I collapsed onto the floor in a mix of exhaustion and relief. I looked at my newborn boy while Susan worked on him. I heard my husband ask with panic in his voice, “Is he okay? Why isn’t he crying? Why isn’t he moving? Is he breathing?” My husband was crying. I, on the other hand, remarked, “Look at all of his hair!” Disoriented from the birth, I didn’t realize that he was still in mortal danger.
My mama eyes saw a beautiful, healthy baby boy. The reality was that my son had an APGAR of 2. He was grayish, limp, had no muscle tone, didn’t cry, and didn’t move. He required resuscitation and immediate transfer. Susan encouraged me to talk to him and touch him to encourage him to breathe as she performed resuscitation maneuvers.
The ambulance arrived and took my baby and my husband to the hospital. I stayed at home with Susan to deliver the placenta, planning to join them later.
The next thing I remember is waking up on my bed and Susan putting something in my mouth; she told me I had lost a lot of blood. I passed out again. The next time I came to, I was on a stretcher, rolling through my front yard in the freezing cold wearing nothing but a sports bra and covered with a sheet. Susan told me that I needed to go to the hospital for blood loss. I stayed awake for most of the ten-minute ambulance ride. I was weak and foggy headed; I felt like I was going to die. I didn’t know where my baby was or how he was doing. I didn’t know if he was alive or if he was going to live or if I would ever see him. I felt numb.
As we rolled through the hospital corridor, I was going in and out. I felt as though I was being dunked repeatedly under water, coming up for air and then going down again. I heard Susan say “Did you hear that?” I struggled to focus, “Hear what?’ I asked. “Eleven two!” I was confused. “Eleven two what?” I asked, bewildered. “Eleven pounds and two ounces! That’s how big your baby is!” It seemed impossible. Had I really just delivered an eleven-pound baby? My sweet boy was almost 4 pounds bigger than his sisters had been.
The OB on call was a compassionate and kind man. He asked Susan exactly what had happened. She shared all the details, timelines, and a rundown of the maneuvers performed. He commended her skillful management. He then examined me, stitched me up, and wished me well. I asked about my son. He said that he was being “worked on” and assured me that someone would send word just as soon as he was stable.
After he left, no one came into my room for a long period of time. I felt forgotten. I was still virtually naked. Bleeding. Cold. Numb.
After an hours-long wait the pediatrician finally walked in with an air of arrogance and declared (without introduction) that our son was going to be life-flighted to the regional children’s hospital. My husband demanded to know, “Why? What is wrong with him? No one has told us anything!” The pediatrician coldly stated, “He is displaying several alarming symptoms. He’s got a ‘thousand mile stare.’ He has absolutely no suck reflex at all. He keeps his hands balled up into fists with his thumbs tucked in. It could be a number of things: seizures, oxygen deprivation, brain damage… I just don’t know. We don’t have the diagnostic equipment or personnel here to properly treat such a complicated neonatal case.” And with that, he left the room.
My son was over five hours old, being prepared to fly in a helicopter to another city, thirty miles away without me, and I still hadn’t held him. I didn’t remember what he looked like. I wanted to see him. My husband tracked down a nurse and told her that we needed to see the baby before he left. She was very kind and brought a wheelchair and a gown (I was STILL naked!) and wheeled me to where he was.
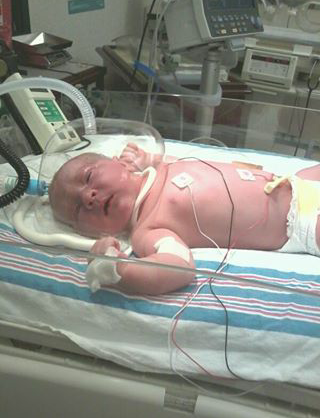
He was massive! Much bigger than I had realized. He was pink now. He had monitor wires coming off of several points on his body and a bubble around his head providing oxygen. I was told that I couldn’t hold him and only had a second because the flight team had arrived. I touched his foot, told him I loved him, snapped a cell phone pic, and I was wheeled away.
I don’t remember when I passed out again, but I awoke to a strange sensation: someone else’s blood being pumped into my veins. It was cold and I could feel it pulse all through my body. I ended up with three bags of blood. After the blood transfusions were complete, I felt like a different person. I was able to sit up without passing out. I no longer feared that I would die. I was too badly swollen to pass urine so they had to catheterize me. How ironic: I had birthed twice in a hospital with no IVs, monitors, medications or catheters. Now, I had received all of the above and more, after my HOME birth!
When was finally released days later I got to Children’s as soon as I could. I walked into my son’s room and sat down by his bedside. I felt so disconnected from him, this baby that I had birthed, but hadn’t gotten to know. I finally got to hold him at nearly three days old. When I held my son in my arms, I cried for the first time. He was real. He was alive. I was alive.
My son suffered from hypoglycemia and had a “rough transition” due to the trauma of his birth. He had limited range of motion (and a gnarly bruise) in the arm that was stuck, but by the grace of God, he had no broken bones. He showed no signs of brain damage after that first day. It was truly miraculous that he came home only four days after his birth.
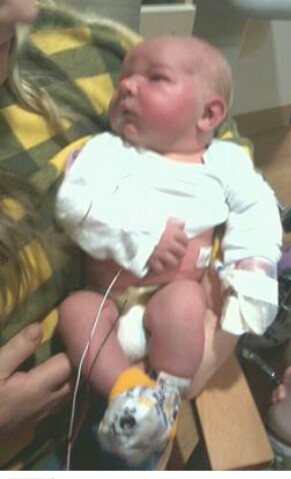 He did require some therapy to gain full use of his left arm, but it rebounded quickly. We were warned that he might suffer from some learning or behavioral issues as he gets older due to his early oxygen deprivation. We were also told to really watch his milestones and development, to make sure to never miss a well-child check-up, and to pay attention to any signs of developmental delay.
He did require some therapy to gain full use of his left arm, but it rebounded quickly. We were warned that he might suffer from some learning or behavioral issues as he gets older due to his early oxygen deprivation. We were also told to really watch his milestones and development, to make sure to never miss a well-child check-up, and to pay attention to any signs of developmental delay.
I am so happy to report that my sweet handsome boy has shown absolutely no signs of any delay or disorder. He has full use of both arms and is as active as any three-year-old boy. He is the light of my life and I thank God every single day for all the miracles that have brought him to where he is today.
Susan and I remain dear friends. She was an absolutely invaluable support to me in the days, weeks, and months after my birth ordeal. I’m thankful that even though I made a questionable choice to birth at home, I was assisted by someone who had the skills and knowledge to help save me and my son, and the compassion to help me through the tough times afterwards.
If I could go back and do it over again, knowing what I know now, I never would’ve attempted to even birth him vaginally, much less at home. But all the decisions that I made back then were made out of genuine care and love. I agonized over every choice and made the ones that felt right to me at the time. I fell right into the same trap that many women do. I believed all the lies: “Your body won’t grow a baby too big for it to birth.” “Birth is as safe as life gets.”
I wasn’t purposely conned or deceived. My midwife didn’t willfully lie to me. She is a wonderful person, who wholeheartedly believed everything that she told me. She is a victim of the same mindset that led me to birth at home, at 42 weeks pregnant, an eleven-pound baby.
If you had told me in 2012 that birthing at home was a poor choice (and many people did), I would’ve argued with you. I BELIEVED in what I was doing. If you had told me that my son was going to be too big to birth safely, I would’ve argued with you. I BELIEVED that wasn’t possible. I was idealistic. I was convinced. I was brainwashed. I was party to a big lie. Now, my eyes are open, but my heart hurts for all the women who will have to sit in a NICU or at a gravesite because they believed the lie.


Does this woman realize that if she had a hospital birth naturally that the same outcome would have occurred? If she had followed her dr’s orders, she would have been induced and/or had a c section and that very well could have caused more problems!?!?!?!?!?!?!?!? I feel for her pain, I transferred from my homebirth and had a c section. It was the most traumatic experience of my life. The staff was horrible, the doctors were cruel. I was literally held down and forcefully put under general anesthesia.
Amber, this woman, who almost lost her baby, wishes she had been under the care of a doctor so that she could have had a safe birth for her child. She states that if she knew then what she knows now, she would have wanted a c-section to keep him safe from almost dying. She still has to live with the fact that he suffered from oxygen deprivation, and if he turns out to have any learning disabilities she will have to wonder if it is due to his birth. She knows that she’s incredibly lucky that he’s a healthy boy now.
Yes, it is possible that a doctor would not have recommended c-section and she could have had a shoulder dystocia at the hospital. But in the hospital her son would have had expert neonatal care immediately available as soon as he was out. Even if it did take the doctor 11 minutes to resolve the dystocia, the baby’s prognosis would have been better at that point. And it probably would not have taken a doctor 11 minutes to resolve the dystocia because they probably would have used McRoberts and suprapubic pressure right away, two maneuvers that she did not list as her midwife having done that are considered standard of care in the treatment of SD.
I’m sorry for your traumatic experience. Trauma is always hard. Tragedy is a lot harder, though. Did it end in tragedy for you? You didn’t mention how everything ended up.
Amber,
Of course she does. Actually, most women choose homebirth because of all the “horror stories” that they hear about the hospitals/obs/doctors/nurses. But then when a horror story happens at HOME, you quickly realize that you do not have the resources that you AND your baby need. You quickly realize that your midwife, no matter how great of a friend she is, she can NOT handle all emergencies. So of COURSE this mother realizes that this could have happened in the hospital as well. But she also realizes that the resources she and her baby needed WERE NOT AT HOME. She’s very lucky that her baby did not die or suffer brain damage. And she’s very lucky that she did not bleed out herself.
How would a C-section have ’caused more problems’? The baby almost died, and might have developmental delays. Instead of the family getting to bond with each other, their new baby was hooked up to various machines and subjected to all kinds of procedures.
If she had been under a doctor’s care, they would have done GD testing which very well could have been a huge factor in her son being so large. If she did have GD and it were properly managed, she may not have ended up with a macrosomic baby to begin with.
She also wouldve likely known that she was expecting a large baby and may have been recommended a section.
Also, she says that she wishes that she hadnt birthed him vaginally at all.
I’m sorry – what? “If she had a hospital birth naturally” the same outcome would have occurred? Sorry, no. At the hospital I birthed at, the OB teams train and hone their skills to make sure they can have a baby safely out in 2 minutes max if things tank. That’s nine minutes less of oxygen deprivation here. They also have a team of neonatalogists already in the room for the resuscitation. My son was also born with an APGAR of 2 after a lengthy vaginal labor in the hospital, nearly 10 lbs. I am so thankful we didn’t have to watch his milestones for social and developmental delays – and I got to hold him almost immediately, and breastfeed right away too.
She stated above that had she known he was over 11 pounds, she would NOT have attempted a vaginal birth. Please read.
Having been in the same as postion …. I would DEF prefer an emergency csec over a 12min sd ……. A csec would of been safer for both mum and baby and far less traumatic emotionally. At least a csec has anesthetisea, my sd had no pain relief while I was held down forceful while they stuck their whole hands right up inside me taking 12min to pull the 12lb baby out …. Who then needed 20min of full resus and emergency transfer to another hospital for specialised neonatal care, not expecting to live the night or possible CP …… Yeah, csec would of been much safer and the more preferred option.
If you were put under general anesthesia after transferring to a hospital from a home birth gone wrong, that means your baby was in so much danger that they didn’t even have time to put in a spinal block or epidural before they did your c-section.
General anesthesia is far and away the fastest way to do a c-section because it works immediately, while epidurals and spinals take 20+ minutes to work. The only reason they would do that is if your baby was in so much danger that they could not wait 20 minutes.
In a situation like that there wouldn’t have been time to get you calmed down and clearly explain to you exactly what was going on. They were focused on saving your baby, since that’s their job and they correctly assumed that you wanted your baby to come out alive and well. I’m sure it was very rushed and very upsetting, but not nearly as upsetting as what would have happened if they hadn’t moved quickly, or if you hadn’t transferred to the hospital.
Amber you are so misinformed. I am a labor and delivery nurse and I have witnessed shoulder dystocia. The difference is the availability of IMMEDIATE neonatal care upon delivery. Please keep your ignorant uneducated opinions to yourself. Birth is and has been one if the mist dangerous things a mother and baby can go through.
I’m so glad this baby and mother ended up OK. But while I’m grateful “Susan” had the skills to resolve the crisis at hand, I pray that she’s learned from this and no longer allows herself to have to squeeze a 11 pound baby out at 42 weeks. Really, how could she not have known that this baby was too big to be born at home? That reeks of dangerous irresponsibility to me. The next giant of a baby might not be so lucky. If “Susan” doesn’t insist on tests and ultrasounds, how is she to know that it won’t be a 12-pounder beforehand and not like “Oops!” at home?
You are completely right Amazed.
I had my 11 pound baby at home in 2012 as well, he suffered from shoulder dystocia and though the midwives applied themselves frantically to all the right maneuvers he was not freed in time and would ultimately die later that week.
I feel like my midwives really DID do everything they could to resolve the dystocia and to get him out. But I am left wondering… did they not notice he was quite macrosomic, or did they notice and just not worry??
They had been measuring and palpitating my belly of course, but I had no 3rd trimester scans.
I was only 40 weeks.
I’m so sorry about your horrific loss. Do you have a copy of your records? Did they make any indications of an estimated fetal weight or any notes about the baby feeling large? Did your fundal height measurement exceed 38cm?
I’m so sorry, Dhanya. You’re Shridam’s mom, right? I remember reading your story and thinking that midwives looked like they knew what they werre doing – but it’s like a life-guard left to guard a single child at the pool and wandering off to buy a beer leaving the toddler there despite the child wanting to go in there on his own and expressing it most vocally. Sure, life-guard might save the child later – but it doesn’t make the decision to left him or her unattended right. And sometimes, they cannot save the child. Like what happened to you.
You make a good point, Amazed. The dangers of skipping prenatal testing (or just as bad, having inadequate testing performed by someone who doesn’t know how to appropriately administer the test or interpret the results) are serious.
Depending on the state, she may not have had the option to order tests or ultrasounds or such. Some states dont grant those rights to home birth midwives.
That’s true, Lauren.
Midwives tend to downplay the importance of services that we can’t provide. Women need to know that these tests are important. If you have chosen a midwife who isn’t able to get you medically necessary tests, you might want to rethink your strategy.
Has anyone mentioned to this mom that based on the size of the infant, the shoulder dystocia, and the fact that the infant had issues with blood sugar postpartum, she possibly (likely) had gestational diabetes and needs to have her A1C checked? She would have had GD testing (or at least been offered it and adequately counseled) if she’d gone with a hospital provider.
Would this still be recommended even though this birth happened three years ago?
Yes, because she is at higher risk for developing type 2 diabetes. The A1C is diagnostic for that.
Thank you, I’ll pass the recommendation along!
I’m so glad that the baby survived this. My brother and his wife had an almost identical homebirth story, except that my sweet niece died. It will be six months this weekend, and not a day passes that they don’t wish they had gone with a CNM in the hospital or the OB that their friends loved. The most hurtful thing has been the hardcore homebirthers who tell me when I share their story that being under the care of an OB at the hospital would have been worse (pretty sure my SIL would have rather had a c-section and a live baby than a 24+ hour labor, massive tearing, and a dead baby).
It is really hard to imagine a scenario worse than what happened. It defies belief that people would say such cold and clueless things to you. I’m so sorry for the loss of your niece.
I also wonder what the CNM care in this mother’s hospital births was. I mean, no monitoring even? To this layperson, it looks like she could have just as well stayed at home because the CNM used “other ways of knowing” anyway.
Now, on a serious note: Leigh, what can a hospital birth with no IV and monitoring (to my lay mind, that’s the bare minimum that should be offered) offer in the terms of safety? How is the medical personnel supposed to tell when things are going wrong?
I say that my hospital birth had “no interventions,” but I’m not including monitoring as an intervention. I would assume that the CNM referred to in this story did monitor the baby.
I have never seen a woman refuse all monitoring. If someone did, then this would considerably reduce the safety of her birth no matter where or with whom it was taking place. However, there is still more safety afforded to the baby born in a hospital because the necessary personnel and equipment for a full resuscitation (including intubation) is near at hand. In addition, hospital-based providers have seen hundreds more births than your average CPM, and would have more education and practical experience in how to, for example, get a baby with shoulder dystocia out faster and with as little damage as possible.
As far as the IV goes, in a hospital setting if the mother starts to bleed out, they can usually put an IV in pretty quick at that time. So although it may be safest to already have an IV or heplock, that doesn’t mean that the benefits of an IV are an entire transport away.
Thanks, Leigh! That makes sense.
I was referring to this part of the story: “How ironic: I had birthed twice in a hospital with no IVs, monitors, medications or catheters. Now, I had received all of the above and more, after my HOME birth!”
No monitors sounded really strange to me but perhaps she meant intermittenr monitoring. I have a hard time trying to imagine a hospital with NO monitoring.
I verified that the CNM used a handheld doppler to monitor her babies’ heart tones. When she said “no monitors,” she meant she didn’t have monitors attached to her.
Hello!
I am the mother in this story. I would like to clear some things up. In my hospital births, I used a CNM who was in a solo practice. When I went into labor both times, I called him directly and he met me at the hospital. In my first birth, I got there first and had to go through triage. The triage nurse had me lay down and put the belts on me for monitoring. She also talked me in to a hepLock after I declined an IV. He got there maybe 10 minutes after I had been hooked up to the monitors. He took them off of me and I never had one on again. He checked heart tones with a handheld Doppler.
With my second birth, he got there before me and met me. I skipped triage altogether and didn’t have the belt monitors on at all. I also didn’t get a heplock or IV. I spent the entirety of that labor in the water, only getting out to push/birth and again only received Doppler checks. In that birth, I bled a little more than he liked so I ended up getting jabbed in the thigh (twice) with shots of pitocin.
So, besides the quick jabs of Pit, nothing was done to me or for me that couldn’t have been done at home (in my mind). My DEM had a Doppler, which is what my CNM used. My CNM had given me a couple jabs of pitocin to stop some bleeding…but putting a chunk of placenta in my mouth wouldve done the same thing (as far as my “research” told me anyway). I even birthed with no coaching, on all fours, on my hospital bed. So you can probably see why I was so confident in thinking that all would go well in homebirthing.
I absolutely can see why you were confident. Once one birth goes well, we think the rest are in the bag. Once two go well, we are total pros! What could go wrong, right? Even as a midwife I pretty much considered my second- or third-timers to be “sure things.” Thanks for commenting!
Thank you Mom for the update, I posted prior without seeing your comment. Please disregard prior post, I’d delete it if I could.
You don’t have to have monitoring or Iv when in hospital! You can birth in hospital with only your mw and nothing else. Just means that if something does go wrong then the help is right there. I had no interventions at all for my second born in hospital. Yet my third had so, was stuck for 12min and 12lbs despite having a full team of medical professionals helping get him out. His a pages were 0,2,2, If we had been at home he would of died.
Amazed, she wasn’t attended by a CNM. She was attended by a homebirth midwife, likely a CPM or lay midwife. Their training is minimal, high school diploma being the ONLY requirement, and they would not be allowed to practice in other countries.
Answer to self: I mean, beyond prenatal tests. I seem to forget that sometimes, those aren’t even offered to homebirth mums.
I declined the had test after never having God before, but did fasting test instead (which still includes blood just not the vomit inducing sugar syrup) and I passed. Yet birthed 12lb baby. Tested afterwards still no gd. Gd isn’t the only reason for large babies
To Mom: Thanks for clearing this up! I can totally see why you thought you’d pass this “test” with swimming colours. When we did something successfully once, it gives us a measure of confidence. Do it twice, and we’re champions!
So pleased you’re both fine.
I cried tears of joy to hear your son survived <3
I've always used a group of CNMs at a hospital and stories like these have helped me to see how I'm good where I'm at and a home birth is just too risky.
I had an 38 wks ultrasound this past Monday to check how big my third girl is since my last was 10lbs 4oz at birth just a few days past her due date. This baby is average on the ultrasound so I feel better that she probably won't be as big. She's probably my last so I really don't care too much if I need a csection so I'm trying not to be too nervous.
I'm grateful for these CNMs that give women another option that is still in a hospital where emergency care can just rush in. Like how they rushed in when my first had meconium and needed suctioning. She only spent an hour in the nicu it seemed to me because she joined me again real quick.
I just want to add my story. My first son was born 9 lbs 10 oz. I had no GD. My son had SD. My epidural failed & the incredible pain in second stage labor forced me to be in the McRoberts position. I was at the hospital, my doctor knew what to do, & still needed to apply pressure to get my son out. He has low APGAR for color, they denied us delayed cord cutting because of his bluish appearance & he suffered a substantial hit to the head resulting in a subdural hematoma that he has to this day as it has calcified. Today is my due date with my second son. He is measuring at high risk doc ultrasound as the same size (& my first son’s ultrasound was off by plus over half a pound). I have been rated as high risk for SD because of specific measurements of the ultrasound, estimated birth weight, & the biggest risk factor of a baby with prior SD & all of my doctors as well as the hospital are pressuring me to deliver vaginally because I’ve delivered a 9 lb 10 oz SD baby with ‘no problems’. I guess they are legally required to offer c section because although it’s offered I am constantly & heavily being dissuaded against it. I have excellent health insurance with a major carrier. My insurance hasn’t been informed in this process so note this is not a matter of insurance covering or not covering. What we are talking about is that medical literature shows that it will cost 9.4 million dollars to recommend prophylactic csections under my circumstances & the risk of permanent injury to my child are 1 in 770. On other words, it’s not cost effective for me to get a c secton & therefore my providers are trained not to recommend it. There’s a lot wrong with obstentrics in this country (the US). They don’t care for you as a person. Their job is delivering a healthy baby & they like their odds. Regardless of what the delivery does to me. Just sharing my story. Please stop shaming mothers on these comments for their decisions. We do the best we can do with what we are presenting & you don’t know the whole story unless you have experienced it. All these people saying she should opt for this or that – the docs didn’t warn her anyway. The docs are warning me & telling me to take what I feel strongly is the wrong course of action. We do our best & these are our decisions, not anyone else’s.
Thank you for sharing your story, Lark. How did everything go with your birth? I hope you and your family are all well!
This article had me crying, just reading the feelings of the mama at the delivery of her baby and the hospital experience. I’ve had shoulder dystocia three times, all of which were in hospital. My most severe one ended in a limp, gray baby, with a room full of staff and panic in the air. The doctor tried all the maneuvers he could, but in the end yanked the baby out of me the same way the midwife in the story did. My baby ended up with a severe brachial plexus injury. Thankfully, he started breathing on his own and didn’t suffer any brain damage. But the experience was quite similar. My next child was born via C-section. I hated every moment of it, but reading this article reminded me why the C-section was really a must and we should be grateful it exists… I always dreamt of the perfect birth, never took any pain meds and having a C-section was the death of all that. But it was also the uneventful birth of my youngest child and for that I’ll be forever grateful.
I had a SD baby back in 2011. She was my first and it never occurred to me I would have anything other than a straight forward labour. My daughter was 8lb 4oz but I am only 5 foot. I was induced but baby would not descend and after being prepped for emergency c-section they decided to go ahead with forceps and she got stuck for seven minutes and was deprived of oxygen for the whole time. I understand ur wish that you had been in hospital, ww had a full operating theatre, midwives, dr and a full paed team. Afterwards a got a full gynae team to stop my haemorrhaging. It was a terrible experience that haunted me, I struggled as a first time mum but did not feel like I could tell anybody how I felt as I was so grateful she was alive. I was an emotional wreck when it came to her first birthday and I tried to deal with how I felt on the minutes that we thought we had lost her. I had an elective section with my second (who I was told would be around 7lb but was 8lb 13oz).
This sounds so very similar to my son’s birth in BC, Canada. I was planning my third home birth with a midwife, but I started measuring too large for dates. Midwife suspected I had undiagnosed gestational diabetes. I had always refused to test based on a midwife’s advice at first birth. Midwives in Canada are all regulated – so I was required to consult with an OB, have my first hospital birth, and also have an OB present at the birth to assist my midwife if necessary. I had a very bad shoulder distocia – had to try several positions & the OB finally stepped in and did the “corkscrew” method, as you described- and birthed a 10lb 4oz baby boy! I am only 4’10” and a very petite frame!! He was also hypoglycemic at birth and had to be treated in the NICU. This and the large birthweight are both due to unchecked gestational diabetes. I have tested positive for it ever since, and have never had these problems again.
For many years women fought hard to have their babies in hospital and the death rate dropped straight away. Now women want this mystical magical birth at home, in a pool where it is completely unnatural to give birth. And when things go wrong they are told to blame the midwife, it is the mother who is to blame. Midwives are taken away from hospitals to accommodate these silly women. I know women have given birth at home since the dawn of time. but people have got teeth pulled at home as well but you wouldn’t demand your dentist come to the house. Home birth should be paid for by the woman.
Annie, are you in the UK by any chance? Since you say that midwives are being taken away from hospitals to attend home births, and since you imply that home birth isn’t being paid for by the women, I imagine you probably are probably speaking of the UK system.
This story is from the U.S. The midwife in this story, like most US home birth midwives, is not being “taken away from hospitals” to accommodate anyone; she is not qualified to work in any hospital. She has no medical credentials. Yet she hangs her shingle, proclaims herself as qualified, and encourages women to pick her to attend their births for a fee. And the mother does pay, in every way, not just financially.
Here in the US, it is all out of pocket. But the midwives who work in the home are not qualified to work in hospitals. They don’t have the same education and training as hospital based midwives.